After a hiatus of a few countries, Thailand once again had an Ashoka presence. With about 80 Fellows elected since 1989, they had enough active ones facing ongoing challenges to keep me occupied. I was connected with a few of their Fellows who needed help moving their organisations forward. One of these was addressing medical negligence and the other two were involved with addressing poverty amongst rice farmers.
I also had the opportunity to attend a couple of farming and community conferences in the North, run a student workshop at a private university, and engage with a project rescuing and rehabilitating street Elephants.
I started in Bangkok with the Thai Medical Error Network.
Fighting Medical Negligence
The Thai Medical Error Network (TMEN) is an informal network of volunteer patients, families, doctors and lawyers across Thailand fighting for the rights of those who have been victims of medical negligence.
Thailand has a very high rate of medical negligence. Between 25,000 and 50,000 patients a year fall victim to serious negligence. Serious repercussions extend from disfigurement to mental and physical disability and death. The long-term impact isn’t just limited to the individual, but to their families too, significantly increasing the scale of people living with the consequences.
The majority of victims fall into the low-income and low literate demographic, whose status means they cannot command the same quality of attention as the rich.
The reasons for the high incidence of negligence appear to split into four primary categories
- Cultural – A bias towards treating Doctors like kings, and a reluctance to challenge treatment decisions based on fear of negative repercussions and further drop in quality of care.
- Personal – Lack of knowledge and awareness of rights, especially among the low income and low literate demographic. Also lack of collective voice and empowerment.
- Regulatory – No legislation or policy supporting the rights of patients or their freedom of access to information about their treatment.
- Systemic – The Medical system protects its own, with strong unions and backup legal support for doctors. Combined with a complete lack of state support systems for patients, the result is that the individual on the receiving end has nowhere to turn.
The overall result is a severe power imbalance in favour of Doctors, and TMEN has been working to change that. When I met them, they were already on the brink of policy change after many years of collective lobbying. The new policy would introduce the safeguarding of patient rights, and enforce medical accountability as well as a state reparation fund for the victims of negligence.
However, getting policy changed is not the same as seeing a difference on the ground. All over the world, there are laws stating rights, but no actual enforcement. This means that the job of a social entity driving change does not end at policy change. Someone has to support and drive the implementation of said change into actual practice.
From Network To Non-Profit
For TMEN to do this on any scale meant needing to raise funds to formalise services, manage the network, disseminate knowledge about rights, create a hub for collection of patient stories and so on. To qualify for funds, needed non-profit status; and to qualify for that required the creation of a formal entity.
Therefore the challenge lay in how to transition a successful non-hierarchical network of volunteers into an organisation with some paid members, without creating the usual pyramid structure or compromising the nature of the open selfless network.
So that’s where I came in. I first met with the main group who managed the network, and together we worked through the whole concept of how to address the challenge, both practically and in terms of organisational design.
They were also keen to understand how to use the web and social media to build audiences and global support, so we had a workshop to demystify and understand how to go about it. What’s super impressive is that today they have a great site up and running using blogger - http://thai-medical-error.blogspot.com/
Then later I worked more closely with the Founder, Preeyanan Lorsermvatta; a fabulous example of selfless drive, perseverance and never-give-up. Preeyanan has been fighting for justice for her son for 19 years. That fight continues, but along the way she has helped thousands others find not just their voice, but reparative justice.
To get to a sensible solution to the problem at hand, we aimed to go through a 5 step process, but really only got as far as step 3 because Preeyanan had other more immediate priorities with driving the impending legislative change.
- Review Problem Definition, Vision, Mission and Strategies
- Lay out a development plan
- Design org structure and operating principles
- Identify resourcing infrastructure and capital needed
- Define transition plan and next steps
Here’s some take-aways for those of you who are dealing with the same problem elsewhere…
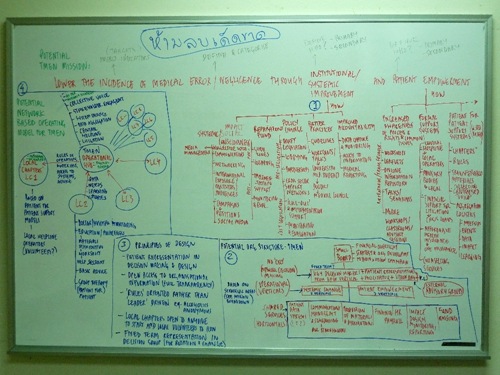
Critical Factors Driving Medical Negligence
Regardless of which country you’re in, addressing the issue of doctor negligence requires addressing the following 8 factors:
Systemic & Institutional Change
- Problem Recognition at a Social and Systemic Level
- Regulatory Policy
- Medical Practices
- Accountability
- Reparation
Patient Empowerment
- Collective Voice and Awareness of Process, Rights and Common Issues
- Informal Patient for Patient Support Systems
- Formal Support Systems (Help-lines, Legal Support, Health Insurance…)
(See the above sketch for a breakdown of how to tackle these)
Trying to create one massive organisation, with branches everywhere never really works. Bureaucracy is a killer. A much better model is a hub and spoke network (also sketched out in the graphic above).
Designing Different
Finally to the most important challenge. Organisational structure. I’ll cover this again a number of times in future posts. It is one of the biggest challenges facing social entities, because having a workable solution is only one part of the equation. Building and designing an organisation that is able to deliver it effectively is the other.
The norm is to copy the commercial pyramidal hierarchy. Here the maximum control and financial value accrues to the ones at the top, ostensibly creating an aspirational ladder of compliance and motivation. From my experience of consulting to some of the world’s biggest companies, I can assure that mostly it just creates bottle-necks and inefficiency.
There are better ways to approach it when the primary motivating driver for participants is not money.
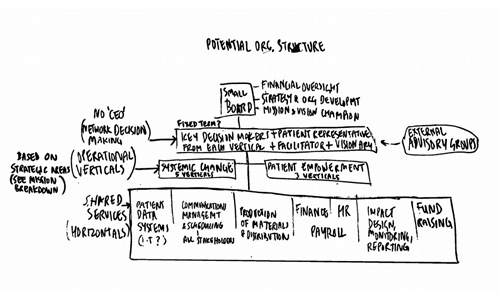
In this case, to prevent losing the networked culture of operating, we had to avoid a structure that created one primary owner / decision maker, and stayed true to the open network culture.
The alternative was to look at a group decision making structure, based on Agile operating principles. This non-hierarchical group would be comprised of representatives from each strategic vertical. Since the majority of those involved in the network were victims of negligence, the issue of patient representation was inherently addressed.
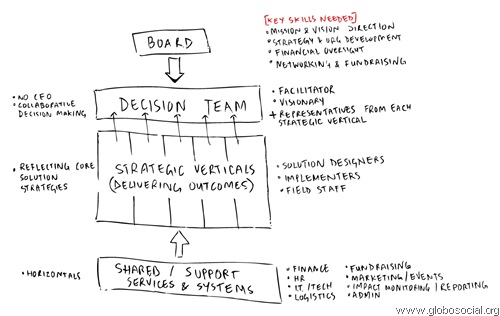
The redesign was loosely based on a model of organisation design that is better suited to ensuring that those at the coalface of helping people make the decisions. The backend functions here provide support and help make things happen, rather then other way round.
I’ll cover more on the underlying model behind this in later posts.
Eradicating Farmer Poverty
Rural Capital Partners is a 20 year old organisation investing in and financing community programmes in Thailand. They’d been working with Organic Rice Farming on a significant scale (6000 tons a year) and were up for an Ashoka Fellowship, so they wanted some help with preparing for their application.
I often get requests to help put proposals together, and I usually ignore the actual proposal writing itself and help the organisation work on the robustness of their solution and operation instead. Anyone can write fancy words and spin out a semantic reality. It’s more powerful when the actuality speaks for itself.
We looked at their mission, strategies and design principles, which led us to review the problem at hand, and consider whether their existing approach would solve it.
The typical approach to helping impoverished farmers is to train them to improve their yield, while also training them on better savings practices.
- There are about 35 million farmers in Thailand, 40% of 15 million of which are below the poverty line. 3 million of these are rice farmers; which straight away indicates the scale of the problem facing any entity trying to eradicate poverty in this sector.
- The second problem is this. The average rice farmer in poverty in Thailand earns about 25,000 baht (about $800) per year, but is typically in debt to the tune of anywhere between 100,000 and 500,000 baht. These loans are typically from loan sharks with crazy interest rates that make them virtually unresolvable for the farmer. Therefore solutions that focus on simply increasing income by a few percentage every year via improving yield, may ameliorate immediate pressures but are never going to solve the long-term poverty cycle.
- The third problem is that cash is not wealth, and simply increasing cash flow to an individual or family does not in any way transform them out of poverty. Wealth is defined by the ownership of assets that hold value; ideally increasing value. So in order to ensure a lasting transition out of poverty, social entities have to consider strategies that create wealth for the people and communities they work with.
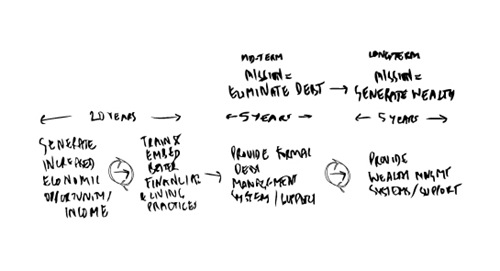
Any solution aiming to eradicate farmer poverty in Thailand, would thus have to extend beyond increasing income and improving savings practices, to debt management and eventually wealth creation systems.
Dealing with Debt
One way to address this kind of debt is to buy it over for the farmer, and then reduce the interest rate down to a manageable level. Ideally just at the point needed to cover the operational costs of providing the service. Think mortgage type repayment terms, except geared towards the benefit of the farmer rather than profit.
The next step would be to formalise savings practices and an investment or banking vehicle to return value on those savings; part of which go towards debt reduction and part of which go towards assets owned by the farmer.
If looked at on a 10 to 20 year timeframe, these kinds of debt and wealth management systems could be super scalable, as proven by micro-finance. This approach could also provide an infrastructure that could be used by other farming and rural development entities; thus establishing a potential to tackle the problem on its actual scale.
Since both these projects were conducted using a translator, it’s been difficult to keep up with progress. This means I’m not sure how much of it was practically implemented in the end, but the concept remains worth considering.


![Some of the many unsolved incidences of negligence in Thailand. [Picture Courtesy TMEN] Some of the many unsolved incidences of negligence in Thailand. [Picture Courtesy TMEN]](http://lh5.ggpht.com/-SXTdLHIaQ4Y/TsYqitO8DcI/AAAAAAAADwk/Z3BaWGy__rY/Unsolvedv1_thumb1.jpg?imgmax=800)